28.06.2018
2.1 Spinal Reflexes
As noted in the previous chapter, a sense of body position is necessary for adaptive motor control. In order to move a limb toward a particular location, it is imperative to know the initial starting position of the limb, as well as any force applied to the limb. Muscle spindles and Golgi tendon organs provide this type of information. In addition, these receptors are components of certain spinal reflexes that are important for both clinical diagnosis as well as for a basic understanding of the principles of motor control.
Myotatic reflex (stretch reflex)
The myotatic reflex is illustrated in Figure 2.1. A waiter is holding an empty tray, when unexpectedly a pitcher of water is placed on the tray. Because the waiter’s muscles were not prepared to support the increased weight, the tray should fall. However, a spinal reflex is automatically initiated to keep the tray relatively stable. When the heavy pitcher is placed on the tray, the increased weight stretches the biceps muscle, which results in the activation of the muscle spindle’s Ia afferents. The Ia afferents have their cell bodies in the dorsal root ganglia of the spinal cord, send projections into the spinal cord, and make synapses directly on alpha motor neurons that innervate the same (homonymous) muscle. Thus, activation of the Ia afferent causes a monosynaptic activation of the alpha motor neuron that causes the muscle to contract. As a result, the stretch of the muscle is quickly counteracted, and the waiter is able to maintain the tray at the same position.
A major role of the myotatic reflex is the maintenance of posture. If one is standing upright and starts to sway to the left, muscles in the legs and torso are stretched, activating the myotatic reflex to counteract the sway. In this way, the higher levels of the motor system are able to send a simple command (“maintain current posture”) and then be uninvolved in its implementation. The lower levels of the hierarchy implement the command with such mechanisms as the myotatic reflex, freeing the higher levels to perform other tasks such as planning the next sequence of movements.
The myotatic reflex is an important clinical reflex. It is the same circuit that produces the knee-jerk, or stretch, reflex. When the physician taps the patellar tendon with a hammer, this action causes the knee extensor muscle to stretch abruptly. This stretch activates the myotatic reflex, causing an extension of the lower leg. (Because the physician taps the tendon, this reflex is also referred to as the deep tendon reflex. Do not be confused, however, between this terminology and the Golgi tendon organ. The myotatic reflex is initiated by the muscle spindle, not the Golgi tendon organ.) As discussed below, spinal reflexes can be modulated by higher levels of the hierarchy, and thus a hyperactive or hypoactive stretch reflex is an important clinical sign to localize neurological damage.
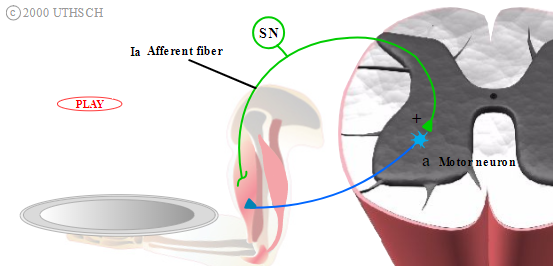
Figure 2.1
Myotatic reflex. This is also known as the stretch reflex, the knee-jerk reflex, and the deep tendon reflex.
Note: Locations of neurons within spinal cord are not meant to be anatomically accurate.
Reciprocal inhibition in the stretch reflex
Joints are controlled by two opposing sets of muscles, extensors and flexors, which must work in synchrony. Thus, when a muscle spindle is stretched and the stretch reflex is activated, the opposing muscle group must be inhibited to prevent it from working against the resulting contraction of the homonymous muscle (Figure 2.2). This inhibition is accomplished by an inhibitory interneuron in the spinal cord. The Ia afferent of the muscle spindle bifurcates in the spinal cord. One branch innervates the alpha motor neuron that causes the homonymous muscle to contract, producing the behavioral reflex. The other branch innervates the Ia inhibitory interneuron, which in turn innervates the alpha motor neuron that synapses onto the opposing muscle. Because the interneuron is inhibitory, it prevents the opposing alpha motor neuron from firing, thereby reducing the contraction of the opposing muscle. Without this reciprocal inhibition, both groups of muscles might contract simultaneously and work against each other.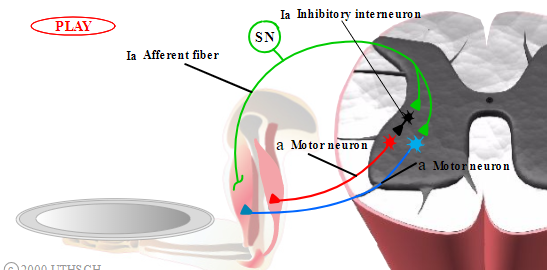
Figure 2.2
Reciprocal inhibition in stretch reflex. Both extensor and flexor motor neurons are firing to maintain the arm at its location. When the pitcher is placed on the tray, the stretch reflex activates the flexor and inhibits the extensor.
Note: Locations of neurons within spinal cord are not meant to be anatomically accurate.
Autogenic inhibition reflex
The Golgi tendon organ is involved in a spinal reflex known as the autogenic inhibition reflex (Figure 2.3). When tension is applied to a muscle, the Group Ib fibers that innervate the Golgi tendon organ are activated. These afferents have their cell bodies in the dorsal root ganglia, and they project into the spinal cord and synapse onto an interneuron called the Ib inhibitory interneuron. This interneuron makes an inhibitory synapse onto the alpha motor neuron that innervates the same muscle that caused the Ib afferent to fire.
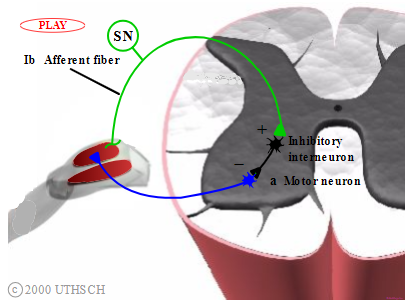
Figure 2.3
Autogenic inhibition. The alpha motor neuron fires to contract the extensor muscle, until the Golgi tendon organ is activated, thereby inhibiting the alpha motor neuron and causing the leg to drop.
Note: Locations of neurons within spinal cord are not meant to be anatomically accurate.
As a result of this reflex, activation of the Ib afferent causes the muscle to cease contraction, as the alpha motor neuron becomes inhibited. Because this reflex contains an interneuron between the sensory afferent and the motor neuron, it is an example of a disynaptic reflex.
For many years, it was thought that the function of the autogenic inhibition circuit was to protect the muscle from excessive amounts of force that might damage it. A classic example is that of the weightlifter straining to raise a heavy load, when suddenly the autogenic inhibition reflex is activated and the muscle loses power, causing the weight to fall to the ground. This function was ascribed to the reflex because early work suggested that the Golgi tendon organ was only activated when large amounts of force were applied to it. More recent evidence indicates, however, that the Golgi tendon organ is sensitive to much lower levels of force than previously believed. Thus, the autogenic inhibition reflex may be more extensively involved in motor control under normal conditions. One possibility is that this reflex helps to spread the amount of work evenly across the entire muscle, so that all motor units are working efficiently. That is, if some muscle fibers are bearing more of the load than others, their Golgi tendon organs will be more active, which will tend to inhibit the contraction of those fibers. As a result, other muscle fibers that are less active will have to contract more to pick up the slack, thereby sharing the work load more efficiently.
Reciprocal excitation in the autogenic inhibition reflex
Just as in the stretch reflex, the autogenic inhibition reflex must coordinate the activity of the extensor and flexor muscle groups (Figure 2.4). The Ib afferent fiber bifurcates in the spinal cord. One branch innervates the Ib inhibitory interneuron. The other branch innervates an excitatory interneuron that, in turn, innervates the alpha motor neuron that controls the antagonist muscle. Thus, when the homonymous muscle is inhibited from contracting, the antagonist muscle is caused to contract, allowing the opposing muscle groups to work in synchrony.
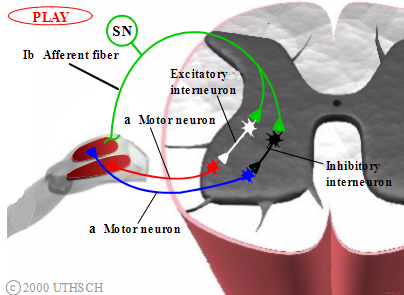
Figure 2.4
Reciprocal excitation in the autogenic inhibition reflex.
Note: Locations of neurons within spinal cord are not meant to be anatomically accurate.
Flexor reflex
Spinal reflexes can be initiated by nonproprioceptive receptors as well as by proprioceptors. An important reflex initiated by cutaneous receptors and pain receptors is the flexor reflex. We have all experienced this reflex after accidentally touching a hot stove or a sharp object, as we withdraw our hand even before we consciously experience the sensation of pain. This quick reflex removes the limb from the damaging stimulus more quickly than if the pain signal had to travel up to the brain, be brought to conscious awareness, and then trigger a decision to withdraw the limb. The reflex circuit is illustrated in Figure 2.5. A sharp object touching the foot causes the activation of Group III afferents of pain receptors. These afferents enter the spinal cord and then travel up the cord. A branch of the afferent innervates an excitatory interneuron in the lumbar region of the spinal cord, which then excites an alpha motor neuron that causes contraction of the thigh flexor muscle. The Group III afferent also continues upward to the L2 vertebra, where another branch innervates an excitatory interneuron at this level. This interneuron excites the alpha motor neurons that excite the hip flexor muscle, allowing the coordinated activity of two muscle groups to withdraw the whole leg away from the painful stimulus. Thus, spinal reflexes work not only at a single joint; they can also coordinate the activity of multiple joints simultaneously.
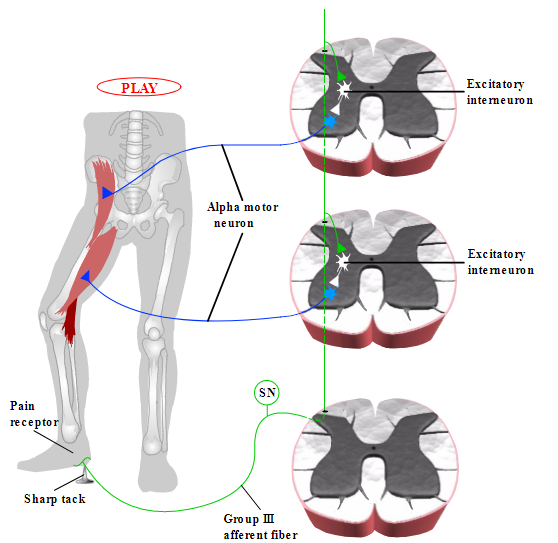
Figure 2.5
Flexor reflex. (Nolte, 2002)
Note: Locations of neurons within spinal cord are not meant to be anatomically accurate.
Reciprocal inhibition in the flexor reflex
When the knee joints and the hip joints are flexed, the antagonist extensor muscles must be inhibited (just as in the stretch reflex). Thus, the Group III afferents innervate inhibitory interneurons that in turn innervate the alpha motor neurons controlling the antagonist muscle.
Crossed extension reflex
Further circuitry is needed to make the flexor reflex adaptive. Because the weight of the body is supported by both legs, the flexor reflex must coordinate the activity not only of the leg being withdrawn but also of the opposite leg (Figure 2.6). Imagine stepping on a tack, and having the flexor reflex withdraw your right leg immediately. The left leg must simultaneously extend in order to support the body weight that would have been supported by the right leg. Without this coordination of the two legs, the shift in body mass would cause a loss of balance. Thus, the flexor reflex incorporates a crossed extension reflex. A branch of the Group III afferent innervates an excitatory interneuron that sends its axon across the midline into the contralateral spinal cord. There it excites the alpha motor neurons that innervate the extensor muscles of the opposite leg, allowing balance and body posture to be maintained.
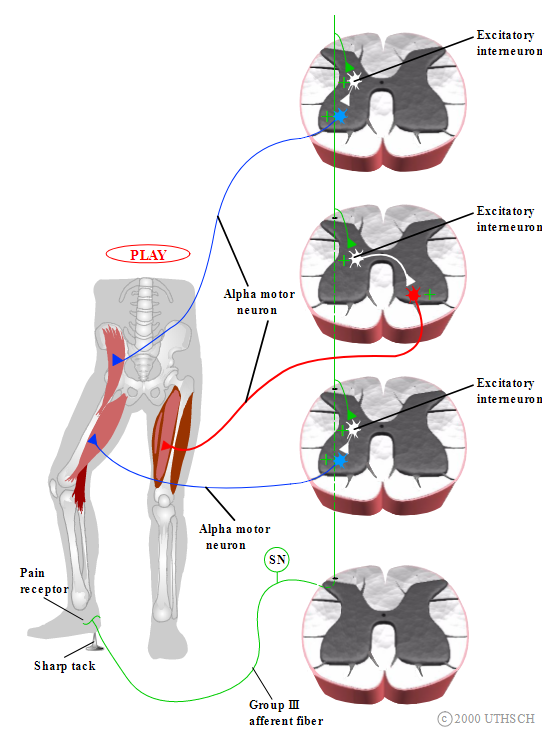
Figure 2.6
Crossed extension reflex. (Nolte, 2002)
Note: Locations of neurons within spinal cord are not meant to be anatomically accurate.
Recurrent inhibition of motor neurons (Renshaw cells)
Axons of alpha motor neurons bifurcate in the spinal cord and innervate a special inhibitory interneuron called the Renshaw cell (Figure 2.7). This interneuron innervates and inhibits the very same motor neuron that caused it to fire. Thus, a motor neuron regulates its own activity by inhibiting itself when it fires. This negative feedback loop is thought to stabilize the firing rate of motor neurons.
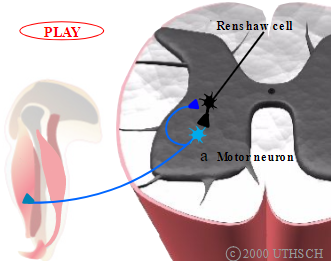
Figure 2.7
Renshaw cell.
Descending Motor Pathways
The reflex circuits demonstrate that sophisticated neural processing occurs at the lowest level of the motor hierarchy. These automatic reflexes can be modulated, however, by higher levels of the hierarchy. For example, when touching an iron to see if it is hot, your flexor reflex may be hypersensitive. As a result, you pull your hand away repeatedly before even touching the iron, anticipating that it may be hot. Conversely, if you remove a hot dish from the oven and the heat starts to go through the oven mitt, you will suppress the flexor response so that you do not drop your dinner as you rush to put it down on a table. These modulations (both facilitatory and inhibitory) of the spinal reflexes arise from the descending pathways from the brainstem and cortex. Voluntary movement and some sensory-driven reflex actions are also controlled by the descending pathways. The corticospinal system controls motor neurons and interneurons in the spinal cord. The corticobulbar system controls brainstem nuclei that innervate cranial muscles.
Parallel and Serial Processing
Although the motor system is organized hierarchically, the hierarchy is not a simple chain of processing from higher to lower areas. Many pathways enable the different levels of the hierarchy to influence each other. Thus, the flow of information through the motor system has both a serial organization (communication between levels) and a parallel organization (multiple pathways between each level). This parallel organization is critically important in understanding the various dysfunctions that can result from damage to the motor system. If the motor hierarchy had a strictly serial organization, like a series of links on a chain, then damage to any part of the system would produce severe deficits or paralysis in almost all types of movements. However, because of the parallel nature of processing, paralysis is actually a relatively rare outcome, produced by damage to the lowest level of the hierarchy. Damage to higher levels results in deficits in motor planning, initiation, coordination, and so forth, but movement is still possible. The parallel nature of organization is also important for the ability of undamaged parts of the motor system to compensate (at least partially) for injuries to other parts of the system.
Descending motor pathways arise from multiple regions of the brain and send axons down the spinal cord that innervate alpha motor neurons, gamma motor neurons, and interneurons. The motor neurons are topographically organized in the anterior horn of the spinal cord according to two rules: the flexor-extensor rule and the proximal-distal rule (Figure 2.8).
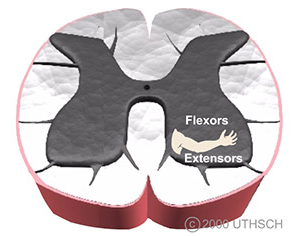
Figure 2.8
Flexor-extensor rule and proximal-distal rule.
Flexor-extensor rule: motor neurons that innervate flexor muscles are located posteriorly to motor neurons that innervate extensor muscles.
Proximal-distal rule: motor neurons that innervate distal muscles (e.g., hand muscles) are located lateral to motor neurons that innervate proximal muscles (e.g., trunk muscles).
Descending motor pathways are organized into two major groups:
- Lateral pathways control both proximal and distal muscles and are responsible for most voluntary movements of arms and legs. They include the
- lateral corticospinal tract
- rubrospinal tract
- lateral corticospinal tract
- Medial pathways control axial muscles and are responsible for posture, balance, and coarse control of axial and proximal muscles. They include the
- vestibulospinal tracts (both lateral and medial)
- reticulospinal tracts (both pontine and medullary)
- tectospinal tract
- anterior corticospinal tract
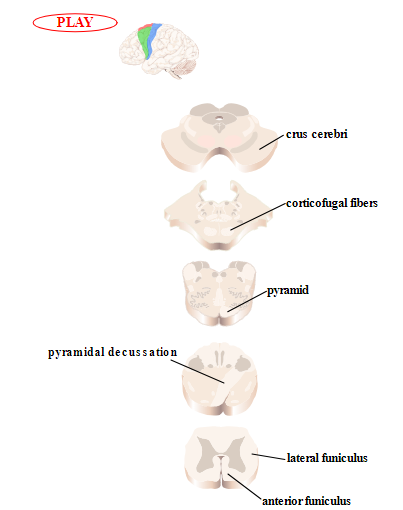
Figure 2.9
Corticospinal tracts (also called pyramidal tracts).
Corticospinal tracts. The corticospinal tract originates in the motor cortex (Figure 2.9). The axons of motor projection neurons collect in the internal capsule, and then course through the crus cerebri (cerebral peduncle) in the midbrain. At the level of the medulla, these axons form the medullary pyramids on the ventral surface of the brainstem (hence, this tract is also called the pyramidal tract). At the level of the caudal medulla, the corticospinal tract splits into two tracts. Approximately 90% of the axons cross over to the contralateral side at the pyramidal decussation, forming the lateral corticospinal tract. These axons continue to course through the lateral funiculus of the spinal cord, before synapsing either directly onto alpha motor neurons or onto interneurons in the ventral horn. The remaining 10% of the axons that do not cross at the caudal medulla constitute the anterior corticospinal tract, as they continue down the spinal cord in the anterior funiculus. When they reach the spinal segment at which they terminate, they cross over to the contralateral side through the anterior white commissure and innervate alpha motor neurons or interneurons in the anterior horn. Thus, both the lateral and anterior corticospinal tracts are crossed pathways; they cross the midline at different locations, however.
Function. The corticospinal tract (along with the corticobulbar tract) is the primary pathway that carries the motor commands that underlie voluntary movement. The lateral corticospinal tract is responsible for the control of the distal musculature and the anterior corticospinal tract is responsible for the control of the proximal musculature. A particularly important function of the lateral corticospinal tract is the fine control of the digits of the hand. The corticospinal tract is the only descending pathway in which some axons make synaptic contacts directly onto alpha motor neurons. This direct cortical innervation presumably is necessary to allow the powerful processing networks of the cortex to control the activity of the spinal circuits that direct the exquisite movements of the fingers and hands. The percentage of axons in the corticospinal tract that innervate alpha motor neurons directly is greater in humans and nonhuman primates than in other mammals, presumably reflecting the increased manual dexterity of primates. Damage to the corticospinal tract results in a permanent loss of the fine control of the extremities. Although parallel descending pathways can often recover the function of more coarse movements, these pathways are not capable of generating fine, skilled movements. In addition to the fine control of distal muscles, the corticospinal tract also plays a role in the voluntary control of axial muscles.
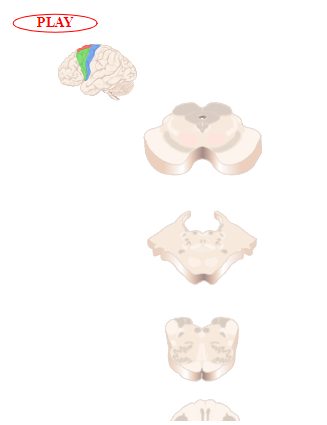
Figure 2.10
Rubrospinal tract.
Rubrospinal tract. The rubrospinal tract originates in the red nucleus of the midbrain (Figure 2.10). The axons immediately cross to the contralateral side of the brain, and they course through the brainstem and the lateral funiculus of the spinal cord. The axons innervate spinal neurons at all levels of the spinal cord.
Function. The rubrospinal tract is an alternative by which voluntary motor commands can be sent to the spinal cord. Although it is a major pathway in many animals, it is relatively minor in humans. Activation of this tract causes excitation of flexor muscles and inhibition of extensor muscles. The rubrospinal tract is thought to play a role in movement velocity, as rubrospinal lesions cause a temporary slowness in movement. In addition, because the red nucleus receives most of its input from the cerebellum, the rubrospinal tract probably plays a role in transmitting learned motor commands from the cerebellum to the musculature. The red nucleus also receives some input from the motor cortex, and it is therefore probably an important pathway for the recovery of some voluntary motor function after damage to the corticospinal tract.
Vestibulospinal tracts. The two vestibulospinal tracts originate in 2 of the 4 vestibular nuclei (Figure 2.11). The lateral vestibulospinal tract originates in the lateral vestibular nucleus. It courses through the brainstem and through the anterior funiculus of the spinal cord on the ipsilateral side, before exiting ipsilaterally at all levels of the spinal cord. The medial vestibulospinal tract originates in the medial vestibular nucleus, splits immediately and courses bilaterally through the brainstem via the medial longitudinal fasciculus (MLF) and through the anterior funiculus of the spinal cord, before exiting at or above the T6 vertebra.
Function. The vestibulospinal tracts mediate postural adjustments and head movements. They also help the body to maintain balance. Small movements of the body are detected by the vestibular sensory neurons, and motor commands to counteract these movements are sent through the vestibulospinal tracts to appropriate muscle groups throughout the body. The lateral vestibulospinal tract excites antigravity muscles in order to exert control over postural changes necessary to compensate for tilts and movements of the body. The medial vestibulospinal tract innervates neck muscles in order to stabilize head position as one moves around the world. It is also important for the coordination of head and eye movements.
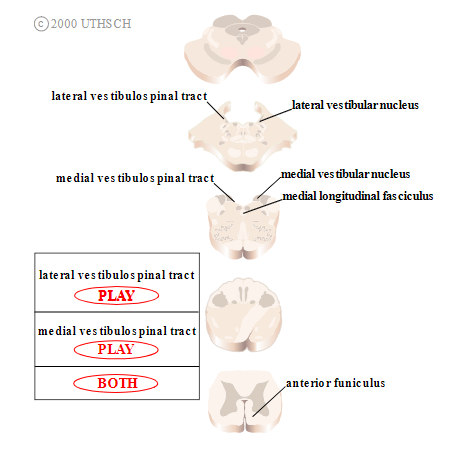
Figure 2.11
Vestibulospinal tracts.
Reticulospinal tracts. The two reticulospinal tracts originate in the brainstem reticular formation, a large, diffusely organized collection of neurons in the pons and medulla (Figure 2.12).
The pontine reticulospinal tract originates in the pontine reticular formation, courses ipsilaterally through the medial longitudinal fasciculus and through the anterior funiculus of the spinal cord, and exits ipsilaterally at all spinal levels. The medullary reticulospinal tract originates in the medullary reticular formation, courses mainly ipsilaterally (although some fibers cross the midline) through the anterior funiculus of the spinal cord, and exits at all spinal levels.
Function. The reticulospinal tracts are a major alternative to the corticospinal tract, by which cortical neurons can control motor function by their inputs onto reticular neurons. These tracts regulate the sensitivity of flexor responses to ensure that only noxious stimuli elicit the responses. Damage to the reticulospinal tract can thus cause harmless stimuli, such as gentle touches, to elicit a flexor reflex. The reticular formation also contains circuitry for many complex actions, such as orienting, stretching, and maintaining a complex posture. Commands that initiate locomotor circuits in the spinal cord are also thought to be transmitted through the medullary reticulospinal tract. Thus, the reticulospinal tracts are involved in many aspects of motor control, including the integration of sensory input to guide motor output.
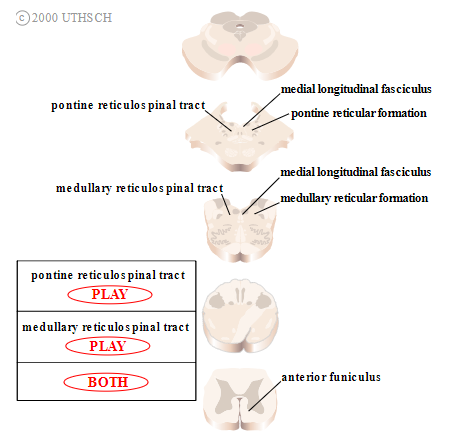
Figure 2.12
Reticulospinal tracts.
Tectospinal tract. The tectospinal tract (Figure 2.13) originates in the deep layers of the superior colliculus and crosses the midline immediately. It then courses through the pons and medulla, just anterior to the medial longitudinal fasciculus. It courses through the anterior funiculus of the spinal cord, where the majority of the fibers terminate in the upper cervical levels.
Function. Little is known about the function of the tectospinal tract, but because of the nature of the visual response properties of neurons in the superior colliculus (the optic tectum), it is presumably involved in the reflexive turning of the head to orient to visual stimuli.
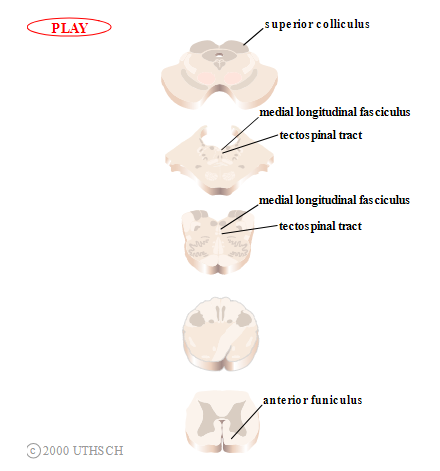
Figure 2.13
Tectospinal tract.
Influences of Descending Pathways on Spinal Circuits
Voluntary movement. The most distinctive function of the descending motor pathways is the control of voluntary movement. These movements are initiated in the cerebral cortex, and the motor commands are transmitted to the musculature through a variety of descending pathways, including the corticospinal tract, the rubrospinal tract, and reticulospinal tracts. How voluntary movements are initiated and coordinated by the motor cortex is the subject of the next chapter.
Reflex modulation. Another critical function of the descending motor pathways is to modulate the reflex circuits in the spinal cord. The adaptiveness of spinal reflexes can change depending on the behavioral context; sometimes the gain (strength) or even the sign (extension vs. flexion) of a reflex must be changed in order to make the resulting movement adaptive. The descending pathways are responsible for controlling these variables. For example, consider the flexor reflex under two conditions.
- Imagine a situation in which you want to pick up a dish from the stove top, but you are uncertain whether it is hot or cold. You may attempt to lightly touch the surface, and this will often lower the threshold of the flexor reflex, making you more likely to pull your hand away even if the dish is not particularly hot. (You may even withdraw your hand numerous times before even touching the dish!) Descending pathways have lowered the threshold for producing the reflex in this case, making it easier for a weaker nociceptive input to trigger the reflex; these pathways can also change the gain of the reflex, making the withdrawal response greater than usual.
- Imagine now picking up the dish in order to move it to the table. As you hold the dish, more of its heat begins to transfer to your hand, and it starts to get quite hot. Rather than dropping the dish and spilling your dinner all over the floor, you rush to the table to put it down, before withdrawing your hand and wishing you had used an oven mitt. In this case, the descending pathways inhibited the flexor response.
Gamma bias. Recall from the previous chapter that there are two types of spinal motor neurons. Alpha motor neurons innervate extrafusal muscle fibers, which provide the force for a muscle contraction. Gamma motor neurons innervate the ends of intrafusal fibers and help to maintain the tautness of muscle spindles, such that they are sensitive to changes of muscle length over a wide range. In order to work adaptively, the activity of alpha and gamma motor neurons must be coordinated. Thus, whenever motor commands are sent by descending pathways to alpha motor neurons, the appropriate compensating commands are sent to gamma motor neurons. This coordination of alpha-gamma motor commands is called alpha-gamma coactivation, and the adjustment of spindle sensitivity by gamma activation is called gamma bias. Consider the following two examples:
- When a command is given to a muscle to contract, the muscle spindles become slack, thereby making them insensitive to further changes in muscle length. To compensate for this, the gamma motor neurons that innervate these intrafusal muscle fibers are activated in concert with the alpha motor neurons, allowing the intrafusal fibers to contract with the muscle. This preserves the sensitivity of the muscle to unexpected stretches of the muscle.
- When a muscle contracts, the antagonist muscle is stretched during the movement. An obvious problem arises when one considers the stretch reflex of the antagonist muscle. If contraction of a muscle causes the activation of the stretch reflex of the antagonist muscle, the antagonist muscle will contract to resist the movement of the limb. How is it possible to ever flex a joint when the stretch reflex of the extensor muscle causes it to extend the joint instead? Alpha-gamma coactivation solves this problem by relaxing the contraction of the intrafusal fibers of the antagonist muscle, allowing the muscle to be stretched without triggering the stretch reflex during a voluntary movement.